The fall
At the end of January, I head up to Bologna for my third post-op check-up. The news isn’t good: I’ve developed a nonunion. It’s a slightly misleading term orthopaedic surgeons use when a fracture just doesn’t heal.
In simple terms, my tibia isn’t healing.
The surgeon doesn’t suggest any treatment—at this stage, the risks would outweigh the benefits. If it turns out to be an infected nonunion, the infection could spread into the bloodstream and cause far more serious damage. Better to let sleeping dogs lie, for now. I walk out of the Rizzoli Orthopaedic Institute feeling hollow. I stop in the Giardini Margheritaand break down in tears.
That’s when it hits me: this is going to be a long tunnel, much longer than I’d expected.
Meanwhile, the pain in my leg keeps getting worse. I go back to using crutches. In March, I decide to get other opinions. I can’t accept that this is how it ends—there has to be a way to rebuild the tibia. I take a train to Milan. At the IRCCS Galeazzi Orthopaedic Institute, they agree with Bologna. But at the Policlinico San Donato (Gruppo San Donato), they suggest a two-stage approach: the Masquelet technique, which I’d already heard about.
The first stage involves replacing the “dead” bone with a cylinder of antibiotic-loaded cement. The body reacts to this foreign material by forming a vascularised membrane around it. After about eight weeks, that membrane becomes a sort of chamber for the final bone graft, taken from the hip.
They’re clear, though: it’ll be a long road (the first surgery won’t be before summer), and my leg will never be the same as it was.
I feel drained—but at least now there’s a sense that something can be done.


The next day, the professor calls me.
“I’ve seen your PET scan. Your situation is a mess. The report is inconclusive. The infection is there and it’s widespread. The only option is Ilizarov.”
My world collapses. The Ilizarov method is the one I’ve been dreading the most. It means living with an external fixator for more than a year.
He adds that waiting times in the public system are too long, and that the surgery would have to be done privately. The cost: €15,000. I haven’t received a single euro since the accident. Negotiations with Grab Holdings and the driver are frozen until I return to Bali. And I don’t feel like asking my parents for money for a procedure I should be entitled to through the public system.
I spend entire days in bed. I don’t want to see anyone.
Then I react, but in the wrong way. I keep avoiding the problem. I surround myself with friends, go out, go to parties. I do everything I can not to think about the sword of Damocles hanging over my head. Meanwhile, the pain keeps getting worse, and I start noticing a white bump on my leg. All the orthopaedic surgeons agree: it looks like a draining fistula, likely coming from the bone.
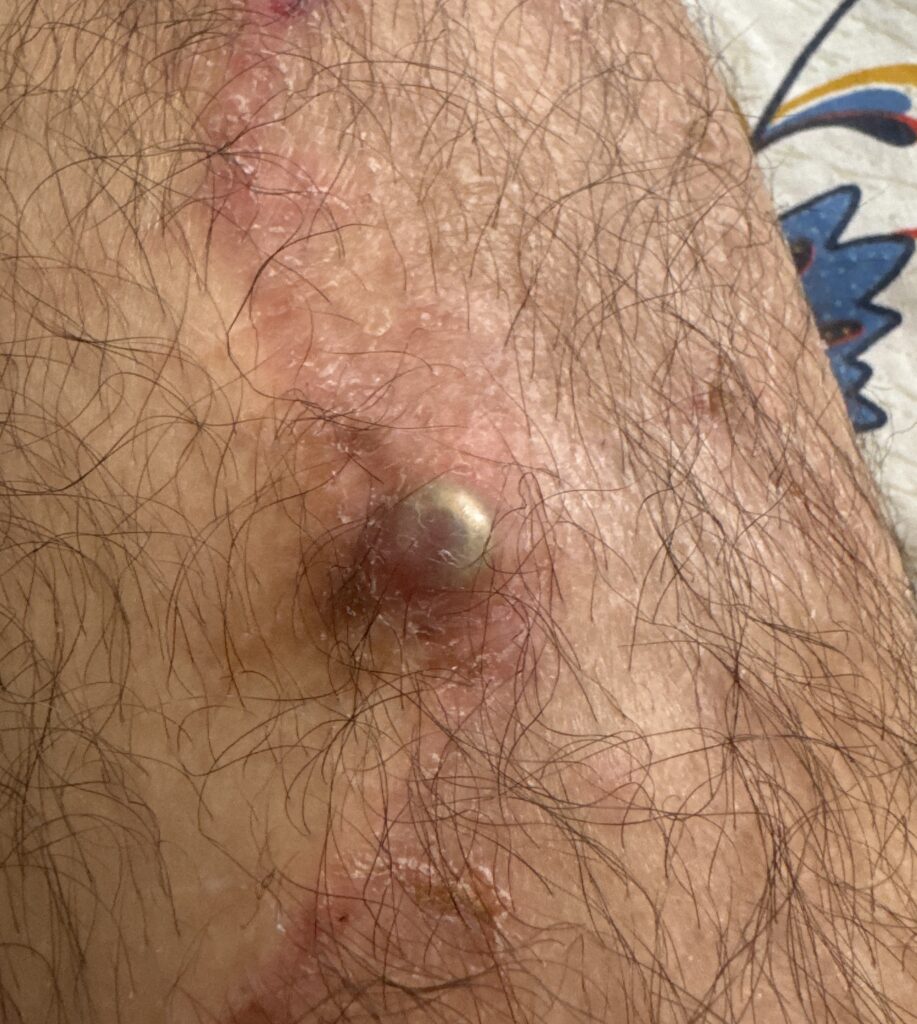
But one night, I shine my phone’s flashlight on it—and I see something strange. A serial code, faintly visible under the skin.
I think I’ve lost my mind.
I start searching on Google and ChatGPT. And then it clicks: that small, round bump isn’t pus. It’s a screw from the plate they put in during surgery in Indonesia. It’s come loose and it’s slowly working its way out, right through my skin.
I pack a backpack in less than twenty minutes and head to Milan. Before going to the ER, I stop at a 24-hour Burger King near the Policlinico di Milano. Somewhere between bites of a burger, I change my mind: I’m not going to Sforza. I’ll go to the CTO Gaetano Pini instead. Online, it seems to be one of the best places for complex trauma cases like mine.
The doctors immediately understand that the situation is serious, but not urgent enough to admit me right away. The head of department wants to see me. He tells me the tibia isn’t in terrible shape. Maybe it’s enough to remove the loosened plate and replace it. In the same surgery, he could also free up my knee, saving me from a separate operation months down the line.
I’m thrilled. Two birds with one stone.
A week later, I’m already in the operating room. When I wake up from anesthesia, they give me the bad news: the tibia wasn’t in as good condition as it seemed. They had to perform the first stage of the Masquelet procedure. Exactly what had been suggested at Sforza. The second stage will have to come months later.
Part of me expected it. I can live with that. It’s only a partial disappointment, because on the knee side, the surgery is a success. In the OR, they reached a range of motion of 120 degrees. I can hardly believe it. The stiffness in my knee had become an obsession. In the previous months, I couldn’t sleep from the fear that I’d never get back to doing simple things like standing up from a chair, walking downhill, or climbing stairs.
The post-op period is tough, but on the ward I meet people with stories a lot like mine. Every day, we gather on the fire escape on the third floor, sharing pieces of our lives. We keep each other going.
I start the summer with cautious optimism. I feel like I’m on the right track.
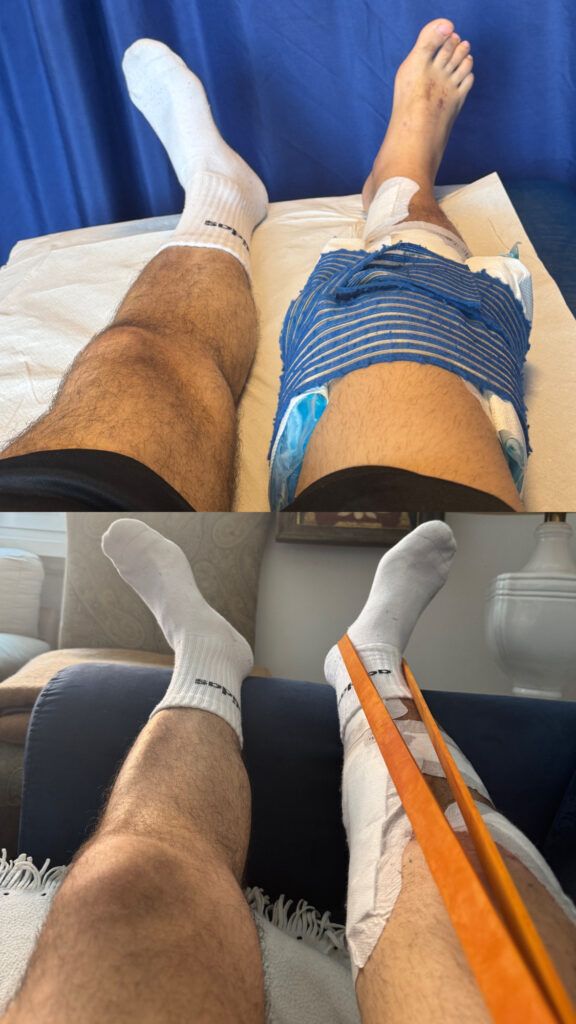
But reality catches up with me soon enough. Even with daily physiotherapy, I can’t get my knee past 60–70 degrees of flexion. The surgical wound won’t close. It keeps leaking, becoming more and more irregular, until it turns into a fistula.
In mid-July, I go back to Milan for a check-up. They tell me the second stage of the Masquelet will have to wait. First, they want a clearer picture of the tibia. More tests. Another appointment, at the end of the summer.
The Roman chapter
When I set foot back in Rome, something feels off. At first, it’s just a deep exhaustion, one that sleep and coffee can’t shake. Then come the chills, and a kind of mental fog. I check my temperature: 38.5°C. There’s no time to go back up to Milan. I rush to the ER at the Policlinico Umberto I, where my friend Giorgia joins me.
The blood tests leave no doubt: it’s the onset of sepsis. The infection is spreading into my bloodstream.
I’m afraid of dying again.
The anniversary of the accident is approaching. A thought starts to take hold: maybe I did something wrong. Maybe the universe gave me a second chance, and I wasted it. Now death is coming back to settle the score.
They put an oxygen mask on me, start IV antibiotics and paracetamol three times a day. On July 24th, exactly one year after the accident, the surgeon tells me there’s no alternative.
Ilizarov is the only way to avoid amputation.
But the final decision is mine. I freeze. They assign me a psychologist to help me process everything and sign the consent forms.
I sink into a depressive state. Another summer gone, confined. Twelve months with my leg locked in a cage. I won’t see the end of this tunnel before autumn 2026.
Outside, life goes on. I eat soup in bed at six in the evening and watch the days fade out through the window.
Sunset is the hardest moment.
I cry almost every day.
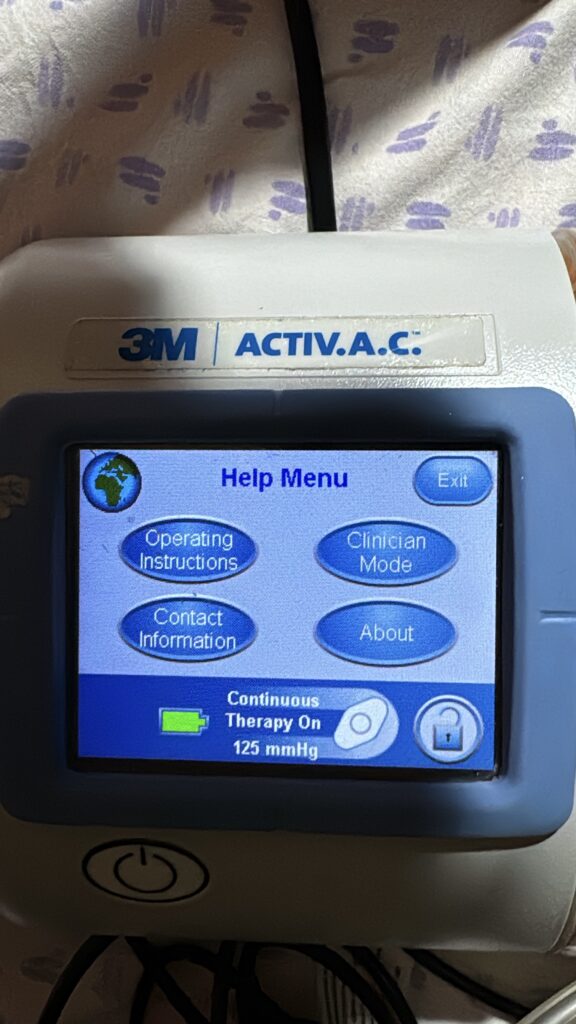
On July 30th, I undergo a first debridement procedure—cleaning out the bone—to take cultures and determine the most appropriate antibiotic therapy. In the OR, they also put me on a VAC: a device that continuously drains fluid from the wound, 24/7. Everyone who’s had one agrees—it’s a nightmare. It’s bulky, and it won’t stop beeping, either because it loses suction or the battery runs low. Even now, I sometimes wake up in the middle of the night, convinced I can hear that alarm going off.
The original plan is to keep me in the hospital until the major surgery in September. But seeing how low I am, the doctors decide to cut me a break. Just before Ferragosto, they discharge me with oral antibiotics and a home VAC.
It’s a kind of conditional freedom. I have to go back to Rome every week for dressing changes. Still, it feels like a fair trade for a small dose of normal life. The summer is lost either way, but it’s better to spend it with my family than in a hospital room.
With a lot of caution, I even manage to spend a few hours at the beach with two friends from high school. I dip my feet in the water.
It’s strange how even the simplest things can shift your mood so completely.

At the beginning of September, the day I’ve been dreading finally arrives. I’m convinced I’m about to undergo the most complex surgery since the accident.
The orthopaedic team will be joined by a plastic surgeon to cover the fistula, using a pedicled muscle flap taken from my right calf (the medial gastrocnemius).
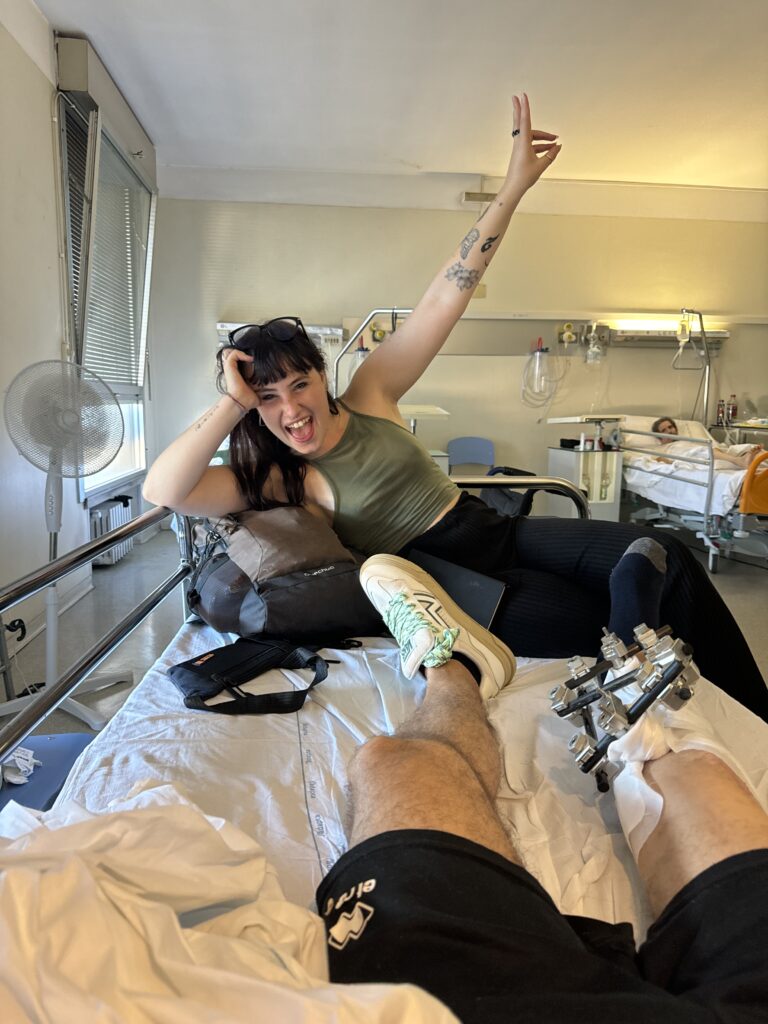
I go into the OR expecting to come out with a circular Ilizarov frame. Instead, to my complete surprise, when I wake up I’m told they’ve performed—once again—the first stage of the Masquelet procedure. They did put on an external fixator, but a monoaxial one, which I’ll only need to wear for a few months, until the second stage of the surgery.
In the middle of an emotional storm, I find myself feeling optimistic.
The intraoperative cultures show an infection caused by S. epidermidis and methicillin-sensitive S. aureus. After eight days in the hospital on IV antibiotics, I switch to oral therapy and can finally go back to Sicily.
Once again, I have to travel to Rome every week for check-ups. It’s not cheap, especially considering I haven’t worked for over a year. But I don’t complain. I’m discovering a kind of inner strength I didn’t know I had.
In October, I move to Milan for a journalism internship at Sky TG24. It’s a glimpse of normal life: I meet new colleagues, build a routine. I feel useful again.
I start to come to terms with my condition. I realize it’s not entirely incompatible with having a life.
It will be a different life, but still one worth living.

Right before Halloween, another blow lands. During my weekly dressing change, the plastic surgeons realize that a new fistula has opened. The antibiotic cement is exposed.
I’m back to square one.
At this point, I don’t even know how I’m supposed to feel. It all starts to feel like some kind of cosmic joke.
At the end of November, I leave Milan, ready to go under the knife again. After a series of delays, a third “first stage” of the Masquelet procedure is scheduled for early December. I’m afraid they’ll have to redo the muscle flap, but instead they manage to extend the one already in place from the medial gastrocnemius.
The surgery falls just a few days before I’m supposed to graduate from journalism school.
Up until the last moment, I hope I’ll be able to attend in person, but I’m not discharged in time. The ceremony ends up being remote, with a very familiar, almost-Covid feel: jacket and tie on top, oversized Adidas pants underneath, to fit the external fixator. I don’t have a laurel wreath, but my friend Martina gives me a virtual one.
That same weekend, two days of celebrations with my classmates are planned. By Friday afternoon, I already have my bag packed, ready to leave, when the final twist comes.
The new cultures show a superbug: a multi-drug-resistant staphylococcus. I’ll have to stay in the hospital for at least another week to set up a new antibiotic therapy. I’m exhausted. I break down, crying from sheer fatigue.
The following Tuesday, they lay out the situation. The standard treatment would mean daily IV infusions for three months. I’d have to stay hospitalized well past Christmas. But the infectious disease specialist manages to get approval for an off-label treatment with dalbavancin. One dose every two weeks, then once a month.
Christmas is saved.
If there’s one strange pattern in all of this, it’s that every setback is followed by some small, almost meagre consolation. Just enough to let me breathe again.
Once more, I go back to Sicily. Once more, I know that every Wednesday night, there’s an Intercity Notte waiting for me.

Another setback. This time, things start going wrong from the very beginning.
The stitches won’t hold. Something underneath is pushing up, putting the whole suture line under tension. A few days before Christmas, they discover an organized hematoma—a collection of clotted blood—under the flap. They remove it and stitch me back up, raw. For a few weeks, it seems to hold, but I have this nagging feeling that, once again, everything is falling apart.
I’m depressed. I spend most of January sleeping, eating sweets, and watching 140 episodes of a Turkish series with my mother.
At the beginning of February, my fears prove right. During a routine dressing change, I feel something hard under my gloves.
I freeze. It’s the cement. Again.
When I go back up to Rome, the doctors don’t really know what to tell me anymore, except that I’ve been incredibly unlucky. We have to start over. Fourth “first stage” of Masquelet. New antibiotic spacer. New flap.
This time, there are no usable muscles left in my right leg. They’ll have to take a free flap from my left thigh—an anteromedial thigh flap.
“This time, it has to work,” they tell me.
It’s the second-to-last bullet to save the leg from amputation. The last one is always there, in the background: Ilizarov. A possibility I don’t even want to think about right now.
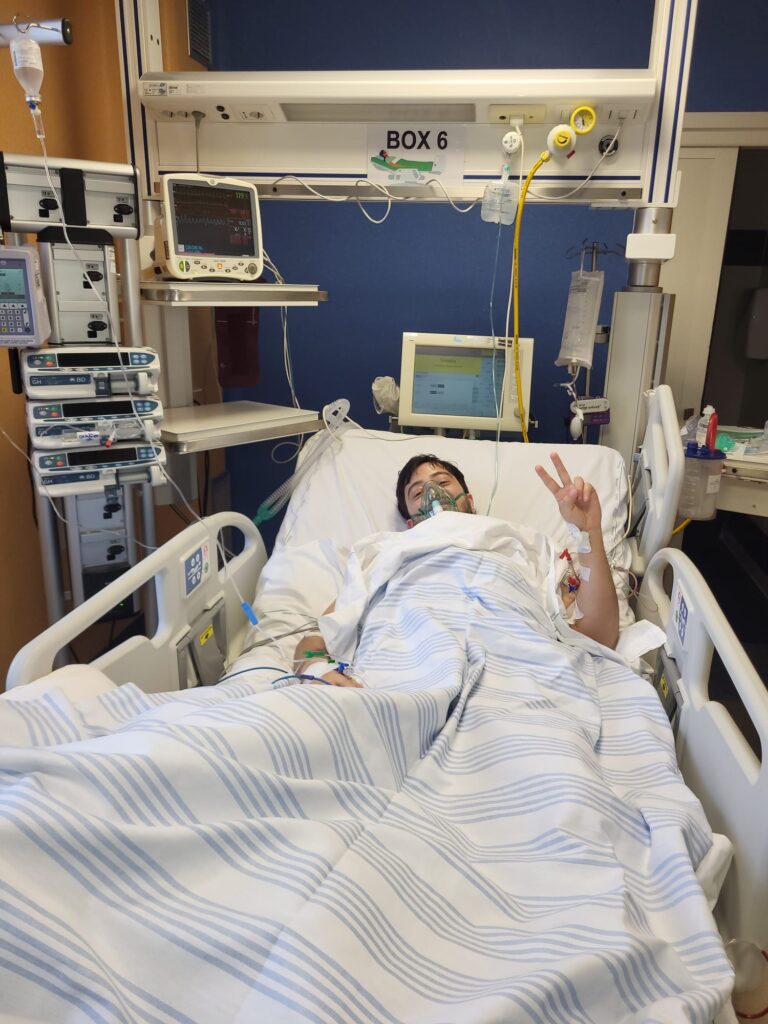
On March 4th, I go into surgery for operation number 7, the longest and most complex since Indonesia. It takes twelve hours of microsurgery to connect the flap’s blood vessels to those at the recipient site. I wake up late in the evening in intensive care, where I’ll spend two days under close monitoring.
Fentanyl. Oxygen. Continuous ECG. I’ve seen this film before.
The first dressing change with the plastic surgeons is brutal. Knowing the theory behind a free flap is one thing—seeing it on your own body is another.
Now I have two disfigured legs instead of one.
I’m extremely weak. It takes me almost a week to recover, two to get out of bed and start walking again with crutches. Nearly a month later, I’m still in the hospital, waiting for the flap to stabilize. If everything goes as it should —and if the infection doesn’t compromise this one too— the second stage of Masquelet is planned for late April or early May.
Surgery number eight.
If the leg is saved, then it’ll be time to think about the knee.
I’ve recently crossed the threshold of one hundred days in hospital.
One hundred days of waking up at six, “good morning, we need to check your blood pressure”, drifting in and out of sleep, “here’s your stomach protector”, half-asleep, “do you want to wash yourself or should we help you?”, breakfast with milk and barley coffee because “they don’t give us real coffee anymore”, “don’t worry, I’ll sneak one in for you”, drifting again, morning rounds, “doc, he’s the patient I told you about, the one who got injured in Thailand”, “Indonesia, I was in Indonesia”, dressing changes, lunch at twelve, “could you empty the urinal, please?”, afternoon slump, jolted awake to start the antibiotics, “the line’s not working anymore, we need to change it”, “how is that possible? You’re so young, but your veins are so hard, we’ll have to try again”, boredom, dinner at six, “same vegetable soup again today”, boredom, Netflix, boredom, “the urinal, please”, insomnia, “who rang?”, “I did, could I have some painkillers? Thanks”, insomnia.
But also one hundred days of kindness and empathy from doctors, physiotherapists, healthcare assistants and nurses. Of sharing personal stories with roommates and residents. One hundred days of my parents bringing me breakfast in bed. Of Giorgia Marelli (they should build that girl a statue) showing up every other afternoon with piadine and supplì. Of friends and colleagues taking turns every weekend, bringing me a bit of comfort, some food, and moral support.
For better or worse, one hundred days. Soon to become one hundred and fifty.
(STORY IN PROGRESS — UNFORTUNATELY)
Meanwhile, the painfully slow pace of orthopaedic treatment doesn’t line up with the timeline of Indonesian justice.
The police are in a hurry to close the case. They want me back as soon as possible to give my testimony. Neither my lawyers nor the Italian embassy have managed to arrange a remote hearing, despite my condition. Flying back and forth to Bali at my own expense seems to be the only way to move forward with the civil case—and hope for some kind of compensation, however small.

An ending yet to be written

I’m sorry to anyone who made it this far hoping for a reassuring ending. This is still a story in progress: even after eighteen months, it feels like everything keeps snapping back to chapter one.
And yet, something has changed since July 24th. Subtly. A quiet form of acceptance is beginning to take hold.
I’m pushing back less. Fighting it less.
I don’t know how many summers will pass before I can swim in the sea again, how many months before I can walk without crutches. How many years before I can go for a bike ride, train properly at the gym, spend a full day hiking. I don’t even know if any of that will be possible, or if it’s just something I cling to so I don’t fall apart completely.
But I do know this: what once felt like a life on hold is, in fact, just a different life, one I’m only now starting to learn how to live with. Over these past months and years, I’ve been surrounded by extraordinary people who’ve shown me what friendship really means. They’ve been there with a plate of pasta, a glass of wine, a walk in the park.
I always say I miss being spontaneous: it’s hard when your independence is so limited. Still, I’ve managed a few small detours. I’ve spent short stretches away from home, met new companions along the way, shared stories.
Slowly, with effort, I’m learning to furnish this tunnel, adding a bit of color to it.
I may not be climbing Everest—nor even the Colli Albani—but I can read, write, make techno music with Ableton Live, improve my German. Even if at a slower pace, less restless than before, I’m still living.
I’m saving my energy for the next leap, whenever life gives me the chance.
To you, reading this—thank you. For your time, and for listening to everything I’ve been carrying inside.
Sharing is the greatest therapy.

